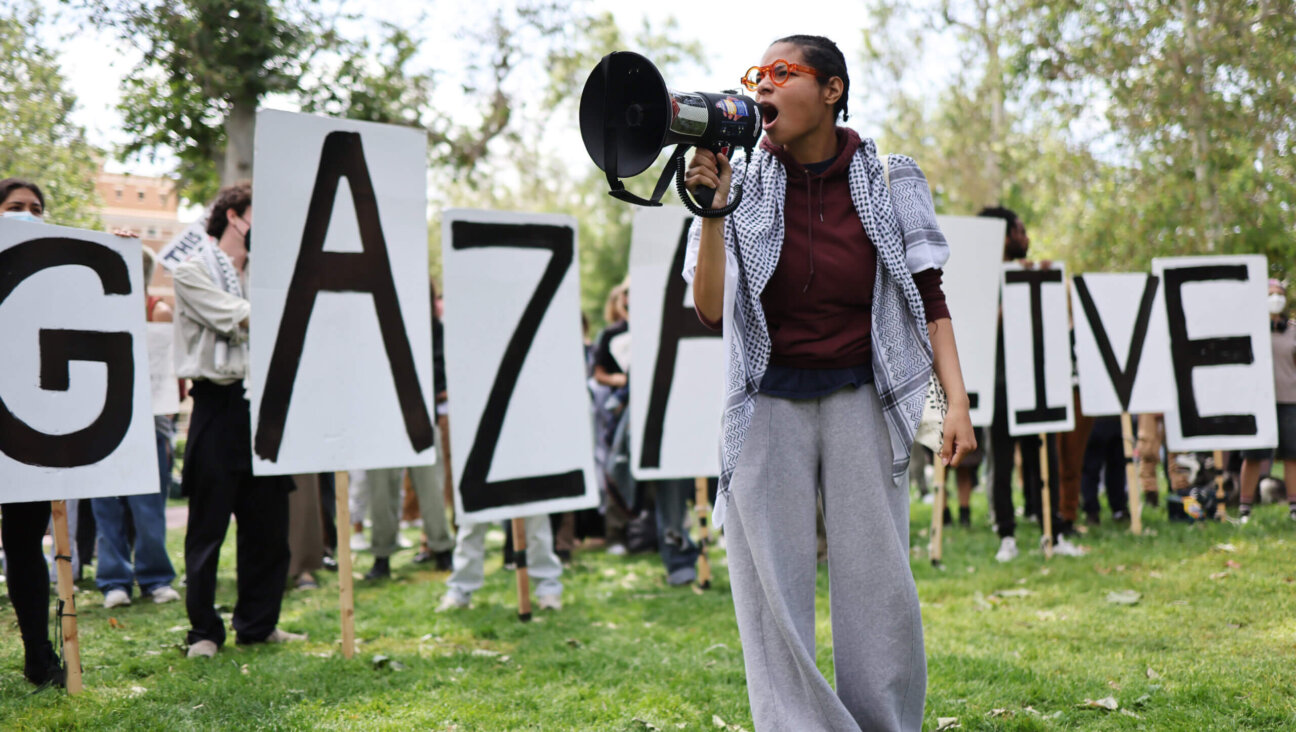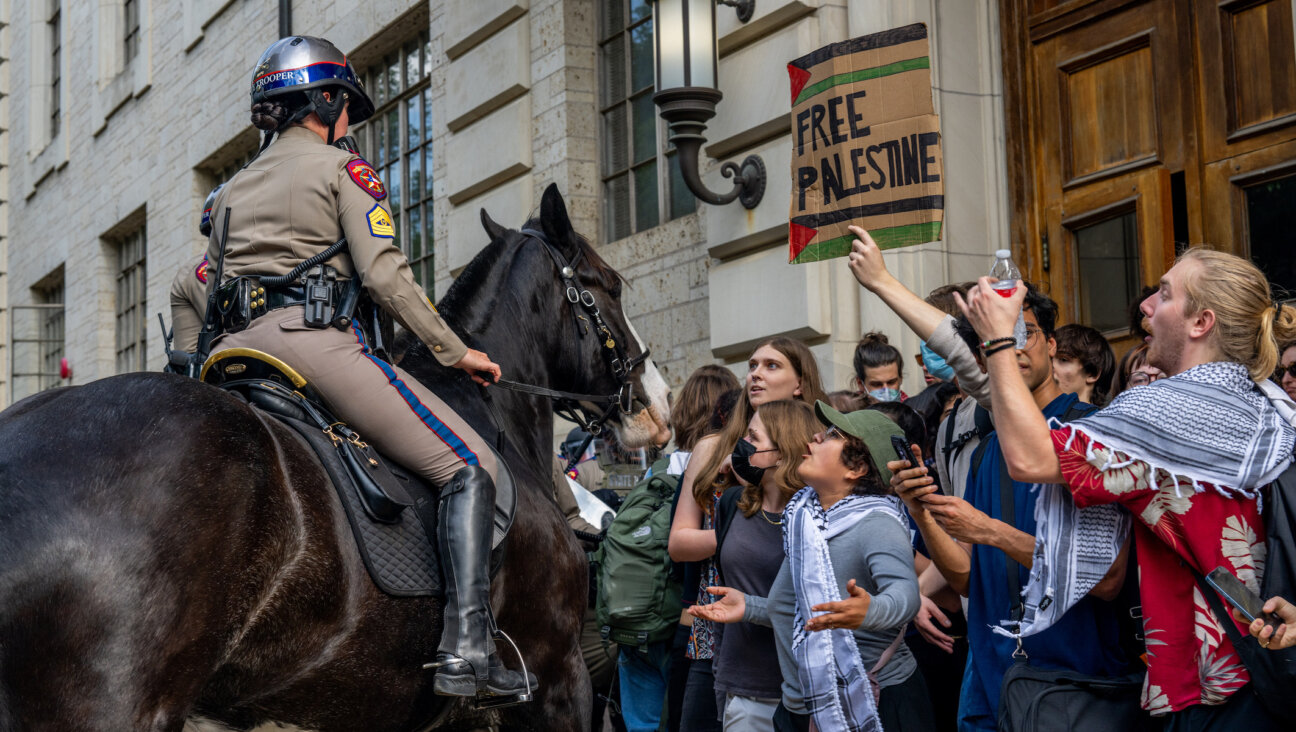A Day in the Life of an Israeli Hospital, Cutting Edge Meets Ordinary Problems

Overcrowded: Rambam struggles to meet demand, with 1,000 beds available for 600,000 oupatient visits every year, giving it an average occupancy of 100.8%. Image by Rambam Medical Center
As the rest of my family spent the day shopping in this picturesque port city on the Mediterranean, I was a few miles away in the hospital — not as a patient, thankfully, but as an observer. In an attempt to learn as much as possible about Israel’s emerging medical technologies, I passed the day at Rambam Health Care Campus, a large government hospital with a renowned trauma center. What I discovered was that Rambam, like many Israeli hospitals, is home to promising new research, but it is also frequently overcrowded and suffers from potentially dangerous physician shortages. What follows is the diary of my time there.
11:07 a.m. After missing the main gate (the entry building was once a German monastery, making it hard to identify as a hospital), my family drops me off at the pediatric emergency ramp. “I wish we could put a GPS on you,” David Ratner, Rambam’s spokesman, tells me by phone. On foot, I take a few wrong turns past the hospital’s medical tourism building and the faculty center for Technion, the technology institute that is contiguous with Rambam, before finding Ratner in front of the Meyer Children’s Hospital. As the sky darkens, patients and visitors — some in hijabs, others in shaytlen, and others still in jeans and T-shirts without head coverings — scurry around Rambam’s campus.
11:15 a.m. Ratner stops at a sculpted model of what the campus will look like when current construction plans are complete. The $250 million effort, which would double Rambam’s surface area, is to include an underground parking lot that can be converted into a 2,000-bed bio-sealed hospital during wartime. Ratner says that the need for the underground facility became evident during the 2006 Lebanon War (when my own cousin dodged bullets while accompanying her husband to dialysis treatments at Rambam).
11:39 a.m. The clouds have broken into rain, and I’m soaked by the time I make my way to the main building. There I meet Shimon Pollack, the yarmulke-clad internist who heads Rambam’s Institute of Allergy, Immunology & AIDS. Some 300 HIV-infected women have given birth to healthy babies under his care.
Last April, Pollack helped start the country’s first Viral IVF clinic, which allows HIV carriers to undergo in vitro fertilization safely, using a single washed sperm cell. (The technology is available, but not widespread, in the United States.) Previously, Israeli couples in which the male partner was infected needed to travel abroad to have biological children. By late January, Rambam’s Viral IVF clinic had resulted in two pregnancies. “The issue of stigma is becoming less and less significant, even in Israel,” Pollack says. “In the early days, some people looked at AIDS as punishment. Not anymore, really.”
12:15 p.m. I’m directed up a staircase and into the temporary home for the Legacy Heritage Clinical Research Institute. There I bump into Derek LeRoith, the endocrinologist who until recently headed the Mount Sinai Medical Center’s Metabolism Institute. He’s a catch, says Michael Aviram, the biochemist and physician who recruited LeRoith. Aviram, best known for writing 450 papers about the health benefits of pomegranates — the ones cited on those attractive POM Wonderful juice advertisements — is now overseeing the building of the Biomedical Discovery Tower. By 2016, Rambam is hoping to have completed the tower and to have recruited a total of 42 researchers in the fields of diabetes, cancer, neurophysiology and cardiology. “The emphasis is on applicable, clinical research,” Aviram says as a ship cruises by on the Mediterranean, outside his window. “They can’t just be in the lab all the time.”
12:45 p.m. In Rambam’s bio-sealed trauma unit, nurses wheel around mobile computers, tending to the victims of a bus accident earlier that morning. In the hall is a small delegation from Israel’s Health Ministry, on a mission to assess a nationwide crisis: hospital overcrowding.
As Israeli-grown medical technology becomes more and more impressive, the country has yet to deal with the very basic problem of overcrowding. A report by Israel’s Health Ministry, released last year, showed that Israeli hospitals are often crowded beyond capacity, so patients are sometimes left out in corridors. And according to a December Health Ministry report, Israel has 1.93 hospital beds for 1,000 people — compared with 2.7 in the United States, 5.7 in Germany and 8.2 in Japan. Rambam has 1,000 beds for 600,000 outpatient visits each year, giving the campus an overall average occupancy of 100.8%. “Rambam, it’s a very modern stable,” Ratner says.
1:11 p.m. The sky begins to clear as I make my way into the small laboratory of Lior Gepstein, a young stem-cell researcher. Scientists in white coats huddle around microscopes, checking on heart cells in petri dishes. “There was an infection over the weekend, so we need to check for survivors,” Gepstein says, referring to surviving cells. Gepstein is best known for being the first person in the world to coax stem cells into becoming heart cells.
Cardiac diseases leave patients with scarred heart tissue. Gepstein has been trying to grow new heart cells that can take their place. After his 2001 paper on deriving the heart cells, the trick became how to get these cells to work with human heart tissue. But the prospect of actually implanting these cells presents two major problems: fear of a rejection of foreign cells and the sheer quantity of these cells required to restore a human heart. Gepstein has also worked with adult stem cells, which can be an answer to the problem of rejection. On the day of my visit, he was waiting for an embargo to be lifted from an article he wrote about converting a woman’s skin cells into heart cells.
2:45 p.m. After Ratner shows me an experiment in the surgical unit — doctors are testing out wristbands that light up if they don’t wash their hands between patients — it’s time to have some lunch and join the rest of my family. This time, we find the main entrance without incident and drive up the mountain, past stirring, bleating ambulances.
Contact Joy Resmovits at [email protected]

I hope you appreciated this article. Before you go, I’d like to ask you to please support the Forward’s award-winning journalism this Passover.
In this age of misinformation, our work is needed like never before. We report on the news that matters most to American Jews, driven by truth, not ideology.
At a time when newsrooms are closing or cutting back, the Forward has removed its paywall. That means for the first time in our 126-year history, Forward journalism is free to everyone, everywhere. With an ongoing war, rising antisemitism, and a flood of disinformation that may affect the upcoming election, we believe that free and open access to Jewish journalism is imperative.
Readers like you make it all possible. Right now, we’re in the middle of our Passover Pledge Drive and we still need 300 people to step up and make a gift to sustain our trustworthy, independent journalism.
Make a gift of any size and become a Forward member today. You’ll support our mission to tell the American Jewish story fully and fairly.
— Rachel Fishman Feddersen, Publisher and CEO
Join our mission to tell the Jewish story fully and fairly.
Only 300 more gifts needed by April 30